Eight Deadliest Superbugs Found Daily in Hospitals
by www.SixWise.com
Every year 48,000 Americans die from a hospital-acquired infection (HAI) -- an infection they DID NOT have when they entered. Increasingly, people are finding that hospitals are some of the worst places to be, as they are literally crawling with germs, some of them “superbugs” that are resistant to antibiotics and other treatments.
In the largest nationally representative study to date, researchers revealed that both sepsis and pneumonia, two infections commonly acquired while in the hospital, are costing U.S. patients a staggering amount in increased health care costs and some are paying with their very lives.
Close to 20 percent of people who developed sepsis after surgery died -- a number made all the more tragic as sepsis is a bloodstream infection that is often preventable. It often occurs because medical equipment is not properly sterilized during surgery.
Many HAIs are the direct result of superbugs … microbes that are becoming increasingly deadly and difficult to treat. Anup Malani, study co-author, investigator at Extending the Cure, and professor at the University of Chicago, said on EurekAlert.org:
"These superbugs are increasingly difficult to treat and, in some cases, trigger infections that ultimately cause the body's organs to shut down.”
Eight Common Superbugs That Could be Lurking in Your Local Hospital
Worldwide superbugs account for more than 2.5 million infections, about 100,000 deaths and billions of dollars in medical costs each year, according to Dr. Philip Tierno, director of Clinical Microbiology and Immunology at the Langone Medical Center at New York University.
What are some common superbugs that could be lurking in your neck of the woods?
1. MRSA (Methicillin-resistant Staphylococcus Aureus)
MRSA kills up to 20,000 Americans each year -- which is a greater death toll than AIDS, which took just over 14, 500 lives in 2007. Not only is MRSA resistant to methicillin, which includes penicillin and related antibiotics, but it's beginning to become resistant to newer antibiotics as well.
If you carry MRSA on your skin without being sick (which happens regularly in about 30 percent of people), you are said to be "colonized" with the bacteria. Though you may not be affected, you can pass the germs on to others.
MRSA typically begins as a skin rash that resembles small pimples, boils or spider bites. The bumps then progress into deep abscesses that may require surgical draining. If the infection spreads beyond the skin, it can lead to infections in your bones, joints, bloodstream, heart and lungs.
2. Resistant Streptococcus (Group A Strep)
This bacteria commonly causes relatively mild illnesses like strep throat and impetigo, but when bacteria gets into blood, muscle or the lungs due to surgery or a wound it can lead to life-threatening, invasive infection, including necrotizing fasciitis (flesh-eating bactiera) and Streptococcal Toxic Shock Syndrome (STSS).
Necrotizing fasciitis destroys skin, fat and muscle tissue while STSS leads to a rapid drop in blood pressure and organ failure. About 20 percent of people with necrotizing fasciitis and more than 50 percent of those with STSS will die.
3. Vancomycin-Resistant Enterococcus (VRE)
Enteroccocci bacteria normally exist in your intestines and in the female genital tract. However, it can cause infections of the urinary tract, the bloodstream or of wounds.
VRE are resistant to vancomycin, an antibiotic typically used to treat enteroccocci bacteria, making them very difficult to treat. This bacteria is often spread from person to person on the hands of caregivers, according to the U.S. Centers for Disease Control and Prevention (CDC), as well as via contaminated surfaces.
4. Resistant Klebsiella Pneumonia
Klebsiella are a type of gram-negative bacteria that can cause pneumonia, bloodstream infection, wound infection and meningitis. The infections are common in health care settings among patients with catheters or ventilators, as well as those taking long courses of antibiotics.
Klebsiella bacteria are spread via person-to-person contact, contaminated medical tools or during surgery. Some Klebsiella bacteria have become resistant to a class of antibiotics called carbapenems, which are typically the last line of defense in treating related infections.
5. Resistant Pseudomonas Aeruginosa
Another gram-negative bacteria, Pseudomonas Aeruginosa is commonly found in soil and water but if it enters your body it can cause infections in your lungs, kidneys or bloodstream. Infections can be particularly deadly in hospitalized patients with cancer, burns, and cystic fibrosis.
6. Resistant E. coli
A new strain of E. coli, ST131, has emerged that is increasingly resistant to fluoroquinolone and other antibiotics. Spread by infected feces that come in contact with food products, the bacteria can cause potentially life-threatening gastrointestinal illness and dehydration.
7. Multidrug-Resistant Acinetobacter Baumannii
Common in severely ill ICU patients or those who have had prolonged hospital stays, Acinetobacter Baumannii can be spread by catheter insertion or other invasive medical procedures. The bacteria have developed substantial antimicrobial resistance, making it increasingly difficult to treat. Mortality rates of associated infections approach 80 percent.
8. C. Difficile (C. diff)
Clostridium difficile is a bacteria that may cause intestinal disease. The bacteria reside in your gut, and most often infection occurs after a person receives antibiotics. Because antibiotics kill both the good and bad bacteria in your gut, it’s easy for C. diff to take over after the course is finished.
C. diff is most common in people who have been in hospitals or other health care facilities, however there is also an aggressive, particularly toxic C. diff strain that has been infecting people who have not been in a hospital or taken antibiotics.
C. diff bacteria is found in feces, and is easily spread from person to person. Because of this, hand-washing and meticulous cleaning are among the best methods to cut down on the spread of infection.
How to Protect Yourself While in the Hospital or Other Health Care Setting
Careful attention to infection-control measures are essential for avoiding superbug infections in hospitals, but data uncovered by the Seattle Times suggests that many hospitals are not following basic procedures like hand-washing.
According to a review of hospital records, the Times found that in some hospitals only 40 percent of staff members wash their hands according to infection-control protocols, and even in the best cases only 90 percent compliance was found. This means that in the best-case scenario one out of 10 physicians, nurses or other health care workers you encounter could have contaminated hands … and often it will be far more.
Doctors’ clothing, from ties to white coats, can also be reservoirs for germs, harboring numerous strains of bacteria that are easily transferred from patient to patient.
This is why if you have a loved one or you are in a hospital, doctor’s office or nursing home we recommend you print off this ”Form To Inform” to help better protect your health.
Again, we highly recommend you print out this “Form to Inform” and give it to all health care workers who you come into contact with to assure they are aware of the risks of superbugs and know you want to reduce your risks of exposure.
Wipe Away Superbugs with PerfectClean Antimicrobial Wipes
Your second line of defense can be PerfectClean Antimicrobial Microfiber hand wipes (used nationwide in hospitals), which will provide an easy way for you to sanitize your hands and your surroundings throughout your stay.
These wipes are used by hospitals, schools and other commercial organizations that require ultra-clean environments. PerfectClean's ultramicrofiber construction combined with a patented antimicrobial chemistry enables these clothes to reach deep into microscopic crevices of all surfaces, including your hands, to remove pathogens in their path ... that is because at an astonishing 3 microns, the ultramicrofibers are even smaller than most bacteria (each cleaning cloth contains over 300 miles of actual cleaning surface!).
PerfectClean products are completely safe, reducing or even eliminating the need for harsh soaps and toxic cleaners. You can use the hand wipes dry or dampened only with water for the most effective clean.
In fact, we recommend carrying a PerfectClean Antimicrobial Microfiber hand wipe in your pocket or keeping one at your bedside and wiping your hand discreetly any time you shake hands or touch a public surface (especially door knobs, food trays, light switches, TV remote control and other heavily contaminated but rarely cleaned surfaces).
PerfectClean Antimicrobial Microfiber hand wipes are made from high-performance hypoallergenic materials knitted with the highest quality conjugated (splittable) micro-denier filaments.
Individual fibers are the same size range (or smaller) than most bacteria. These microscopic fibers are produced by a complex manufacturing process that involves hundreds of variables that splits a polyester-polyamide conjugated filament (bicomponent) resulting in from 9 to 16 microscopic fibers.
Again, these split filaments achieve an individual fiber size of approximately 4-6 microns (bacteria range from 2-8 microns).
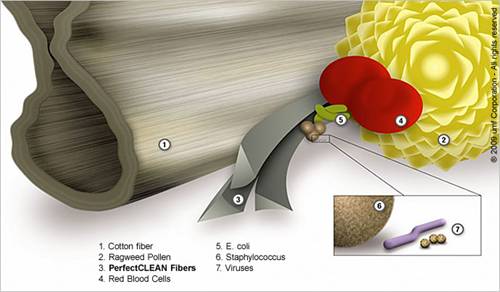
Graphic Size Relationships to PerfectCLEAN Fibers in Antimicrobial Wipes
PerfectClean performance is further enhanced by the material’s overall positive (+) electrostatic charge. In fact, the electrostatic charge developed by a PerfectClean wiper naturally is greater than the electrostatic charge developed by disposable dust sheets chemically.
Dirt and dust particles, bacteria and pollen, and other organic particles all have a negative (-) charge. Thus, PerfectClean fibers literally act as thousands of tiny magnets (positively charged fibers attract negatively charged dust, dirt, etc.) attracting and binding all types of particles.
When damp, fiber quality and quantity provides an enormous surface area within the material, which accelerates and increases wicking of solution through the material resulting in a powerful capillary action (suction) achieving the highest absorption capacity of any material tested.
How to Use Hospital-Grade Microfiber Hand Wipes
- Place in your pocket or purse or by your bedside. Wipe and rub your hands and fingers thoroughly after you come into contact with people through handshakes or when you touch any surfaces that others have touched.
- Clean surfaces using Hand Wipes from your food tray and TV remote to your nurse call button and bed rails.
- Can be used dry or lightly dampened. They are capable of “trapping and removing” 99.99% of bacteria from hard surfaces throughout your home, hospital room, (also your computer keyboard to TV remote control and any workplace).
- Wipe frequently touched areas anytime guests or others (including hospital staff and physicians) visit you.
And because PerfectClean Antimicrobial Microfiber hand wipes are made of highly durable ultramicrofiber cloth, you can use them for 100+ washes before you need to replace them -- making PerfectClean Hand Wipes incredibly economical for everyday use.
Physically removing germs from your hands and environment before they gain entry into your body -- using hand-washing, PerfectClean Antimicrobial Microfiber hand wipes, or both -- is an important variable in staying free from infectious diseases and superbugs.
Also be sure you take advantage of PerfectClean's Total HomePure Pack for all of your home’s deep-cleaning needs.
Includes:
- 2 All Purpose Terry Cloths
- 2 Super Silk Cloths
- 3 Lenstronic Cloths
- 2 Scrub & Clean Reversible Gloves
- 1 Flexible Duster with 2 Duster Covers
- 1 EasyGrip 16"-wide Flat Mop System w/Ergonomic Handle
- 2 Flat Mop Heads
Again, the ultramicrofibers in these products reach into microscopic nooks, crannies and crevices on your floors, countertops, furniture and other surfaces and remove everything in their path. No other type of cleaning tool can come remotely close to removing microscopic contaminants that can make you sick!

SixWise Says ...
Staying out of a hospital is your best defense against getting a hospital-acquired infection. Read How to Eliminate Cures that can Kill for tips to keep you out of the hospital!
Recommended Reading
How to Eliminate Cures that can Kill
New Deadly SuperBug “C. Diff”: Health Warning!
Sources
DailyFinance.com October 17, 2010
Physorg.com July 30, 2010
EurekAlert.org February 22, 2010
Archives of Internal Medicine February 22, 2010; 170(4):347-53
CDC.gov Group A Streptococcal (GAS) Disease
CDC.gov Klebsiella pneumoniae (K. pneumoniae )
The Seattle Times November 16, 2008